The healthcare sector of the U.S. economy is extraordinarily dynamic and complex, providing constant challenges for policymakers and regulators working to improve healthcare markets. However, recent research and policies suggest the greatest challenges for policymakers might be their misunderstanding of economic fundamentals.
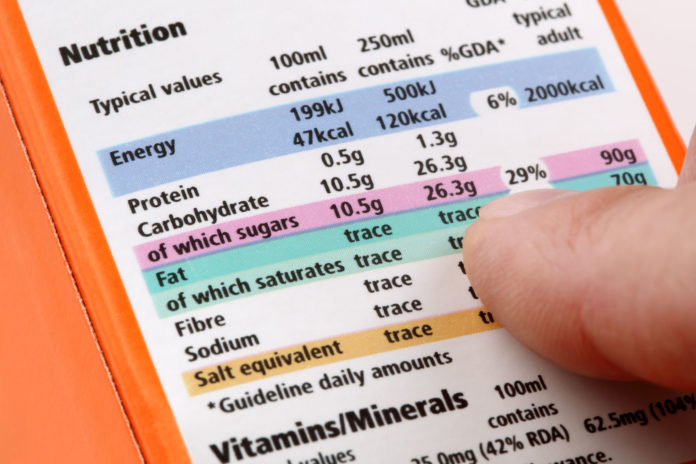
Earlier this year, the Annals of Internal Medicine journal published a paper which found the prices increased for nearly 100 drugs while they were in a shortage between 2015 and 2016. The paper also notes these “price hikes” (price increases) were less severe in markets with comparatively more competitors (defined as more than three drug providers).
Although the authors consider these findings “mysterious,” they confidently offered policy recommendations to correct “the imbalance between supply and demand.” As they stated in their conclusion, “If manufacturers are observed using shortages to increase prices, public payers could set payment caps for drugs under storage and limit price increases.”
The situation described above, and the folly of its policy prescription, are no mysteries for anyone who understands basic economics.